Physician Schedule Optimization Model
Physician Schedule Optimization Model
Use data science and our decades of experience to create a customized physician schedule optimization model. Models like these can help you uncover how your schedules are currently optimized and how changes might improve operational performance.
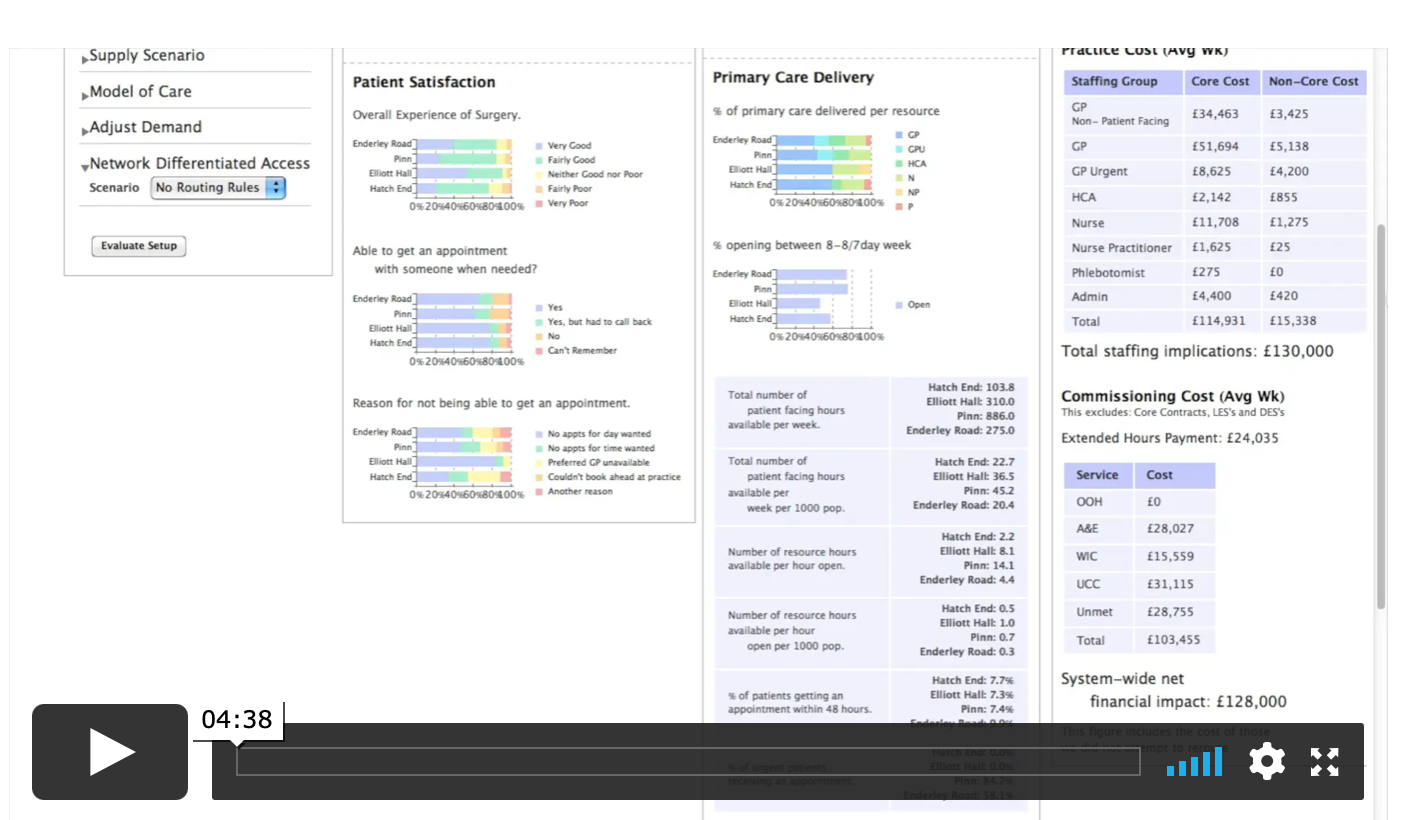
This example of a physician schedule optimization model provides a view into the utility of our approach. Built for a national healthcare system, this physician schedule optimization model illustrates the power of data science and simulation – for both strategic decisions (e.g., adding new resources like physicians or buildings) and tactical choices (e.g., hours of operation).
Let’s Talk
We will help you overcome strategic challenges to realize the business value you seek.